Gastroesophageal Reflux Disease (GERD)
Gastroesophageal reflux disease (GERD) is today the most common disorder of the upper gastrointestinal tract. It is believed that over 20% of the adult population at least once a month has symptoms of GERD, while in 5% of this condition can impair quality of life and can lead to serious complications. The acronym GERD used in clinical practice as a term that encompasses all the clinical aspects of gastroesophageal reflux disease, whether it is related to her symptoms or damage uzorokovana pathological reflux želudačanog contents into the esophagus.
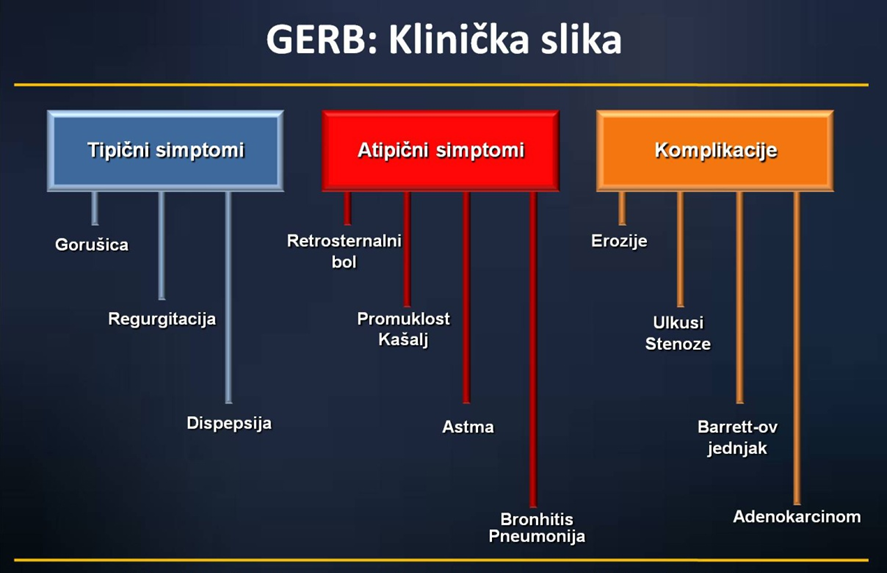
GERD is defined as a set of troublesome symptoms and / or damage caused by the reflux of gastric contents into the esophagus. The clinical presentation of GERD vary, and include typical and atypical symptoms and complications as well, giving the disease a very wide range. In addition to heartburn, or burning sensation behind the breastbone, which is our most frequent symptom of GERD, the patient may feel regurgitation (involuntary return of food and fluids from the stomach into the esophagus), and difficulty swallowing. These three symptoms are typical manifestations of GERD, but a number of other symptoms that do not normally associated with the digestive tract may also be caused by reflux of gastric contents into the esophagus. If the extreme heartburn occurs two or more times a week, can impair quality of life. Such a frequency of heartburn should be a reason to see the doctor, to carry out specialized and adequate diagnosis and treatment. On the other hand, frequent regurgitation especially dysphagia requires immediate medical consultation. Damage to the esophagus, which is associated with GERD are esophageal mucosal inflammation, narrowing of the esophagus caused by stomach acid and Barrett’s esophagus. Finally, as a result of several years of dramatic reflux disease can arise from cancer of the esophagus.
In the last decade, she began to have received increasing attention gastro reflux disease, primarily due to an increase in its prevalence and impact on the quality of everyday life. This heightened focus has been attributed to several factors that can be reduced to the following sentence: GERD is a common problem of modern man, can potentially lead to serious medical complications, and the cost of treatment that include diagnosis, treatment and prevention of diseases are becoming even bigger.
Details about the frequency, reasons for the occurrence, symptoms and potential complications that may arise due to GERD, read below.
Introduction
Gastroesophageal reflux (GER), also known as acid or the acid reflux, occurs when stomach contents back into the esophagus and / or mouth. GER is defined as a retrograde movement of gastric content into the esophagus without strain, and is not a disease but a normal physiological process. Episodes of physiological reflux is javlajaju after meals, short duration, generally do not produce severe symptoms and very rarely occur during sleep. On the other hand, pathological, damaging reflux is associated with symptoms and / or damage to the mucous membrane of the terminal part of the esophagus, often accompanied by episodes of nocturnal heartburn feeling. Acid reflux becomes gastroesophageal reflux disease (GERD) when causes distressing symptoms and / or damage to the esophagus. The term reflux esophagitis mean the group of patients with symptoms of GERD where there is confirmation of endoscopic mucosal inflammation of the esophagus.
Due to the broad spectrum of conditions attributable to reflux, yet there is no real definition of this disease. Generally under GORD symptoms can include patients that indicate the existence of reflux and its complications, but not always with inflammation of mucous membranes of the esophagus (NERD – non-erosive reflux disease). The American College of Gastroenterology (ACG) defines GERD as “symptoms or mucosal damage caused by abnormal reflux of gastric contents into the esophagus.” On the other hand expert consensus, known as the Montreal classification defniše GERD as “a condition that occurs when reflux of stomach contents causes troublesome symptoms and / or complications”. However complications caused by GERD can occur even when the patient is no typical symptoms.
The anatomical and pathophysiological perspective GERD is the inability of normal antireflux barrier to protect the distal esophagus of pathological gastroesophageal reflux. The pathological reflux is characterized by frequent episodes of reflux (> 50 episodes / 24 h), a longer duration (> 3 episodes of more than 5 minutes), with an increased time acidic (pH 4% / 24 h), which may occur during the day and / or night, and can cause the symptoms and damage to the mucous membranes of the esophagus. The amount of acid reflux required to cause GERD is individual. Generally, damage to the esophagus occurs more frequently when reflux is frequent, content extremely acidic, or the esophagus is unable to adequately expel acid out. GERD represents a spectrum of diseases that mainly produce symptoms of heartburn (pyrosis) or regurgitation (regurgitatio), and vomiting, and difficult or painful swallowing. Reflux of gastric contents may damage the vocal cords causing hoarseness or cause inhalation into the lungs (aspiration).
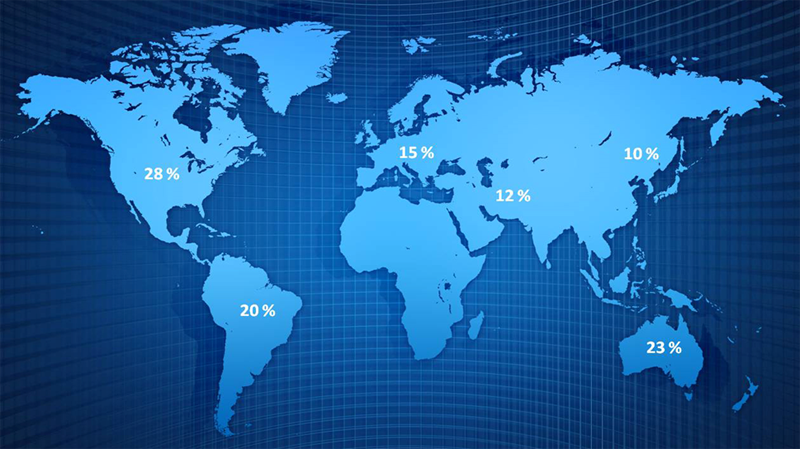
GERD as a very complex process, now represents one of the most common diseases of mankind. The range of prevalence (total number of infected persons in the whole population) of GERD in the world varies significantly. Today it is considered that the prevalence of GERD in North America amounts to about 28%, Australia 23%, Europe 15% (with a range of 9 to 26% with higher in Northern Europe), Middle East 12%, while the lowest in East Asia where only about 10%. Also, there is an evident trend towards increasing prevalence in the US compared to Europe, as well as increasing prevalence in the northern compared to southern Europe. On the other hand, the incidence (number of new patients in a year) in the United States and Europe, the average is 5 per 1,000 inhabitants. Today it is considered that in the Western world about 22% of heartburn or regurgitation at least once a month, while about 16% have a monthly feeling just regurgitation. Endoscopically verified mucosal inflammation of the esophagus (erosive esophagitis) exist in approximately 7% of the population of North America, while in Europe the level of prevalence of the disease varies from 2 to 10%. Erosive esophagitis is present in about 20% of people who have a sense of heartburn at least once a week. It has been shown that the annual incidence of GERD complications increases dramatically after 40-years of age, and that is three times more common in men. Last 30 years the United States has noted the existence of direct opposite correlation incidence of peptic ulcer disease and GERD. While the incidence of duodenal ulcer in the last three decades of the last century has decreased by four times, in the same period, the incidence of reflux disease even increased sixfold and is in exponential growth. At the beginning of the second half of the first decade of the XXI century in Europe about 20 million people suffering from GERD (prevalence of 15%), including all forms of manifestation, with the year only to their treatment spends around € 8 billion.
Causes
When we eat, food is passed from the mouth into the stomach through the pharynx and esophagus. At the lower end of the esophagus, where it continues in the stomach, there is a circular muscular ring called the lower esophageal sphincter (DES). After swallowing, DES is relaxed to allow the food to pass into the stomach and then is collected in order to prevent and restore the food acid in the esophagus. However, it DES becomes weak or relaxes more often because the lower stomach empties and becomes enlarged (distended), allowing the liquid gastric contents to go back up into the esophagus. This process happens occasionally in all individuals. The largest number of reflux episodes occur shortly after a meal, are short and cause short-term symptoms.
The diaphragm is a large flat muscle that separates the chest from the abdomen, and that relaxes and contracts as the patient exhales and inhales. The esophagus passes through an opening in the diaphragm called diaphragmatic hiatus before it continues in the stomach. Normally, collecting aperture enhances the strength of DES, especially during bending, coughing or straining. If there is a weakness in the muscles of inferior level hiatus, the stomach may partially prolapse through the diaphragm into the chest cavity, forming a sliding hiatus hernia (gastric hernia). The presence of a hiatus hernia is a common acid reflux. The exact cause of esophageal hiatus hernia is unknown but may be associated with a decrease in fibrosis and tissue around the diaphragm, which occurs with age.
The initial moment in the development of GERD is an increase incidence of reflux reasons which have not yet known with certainty. The presence of large amounts of acid in the esophagus leads to the emergence of non-erosive esophagitis (inflammation of mucous membranes without damage), which directly affects the functioning of the weakened muscles of the esophagus. The primary manifestations of impaired muscle of the esophagus are reducing the contractility of the internal sphincter, or DES and shortening the total length of the esophagus due to acid-induced contraction of the longitudinal muscle of the esophagus. Reduction in contractility directly leads to a reduction of pressure in DES, while shortening the longitudinal muscle affects the occurrence of fibrosis or permanent shortening and the occurrence of hiatal hernia. Therefore, the formation of hiatal leads to an increase dijafragamalnog opening of the esophagus. The presence of hiatal hernia and weakness of inferior, external, sphincter leads to the formation of additional reflux mechanisms which further enhance GERD and lead to the occurrence of erosive esophagitis, and then severe complications.
Symptoms
GERD is now generally diagnosed based on symptoms, which are common in the general population, especially in people older than 40 years. People who have heartburn at least two to three times a week may have gastroesophageal reflux disease. One of the basic questions related to the issue of GERD, as its impact on quality of life of patients themselves. It is an interesting study which showed that the quality of life in patients with GORD extremely disturbed and that is similar to or even lower quality than in patients with arthritis, myocardial infarction, weakened heart beat or hypertension. Najznačjaniji symptom of GERD, heartburn, is experienced as a feeling of burning, burning behind the breastbone, which occasionally spreads to the throat and can lead to sour taste in the mouth.
| Symptoms of GERD |
|---|
| Heartburn |
| Regurgitation of food / liquids, acid taste in the throat |
| Chest Pain |
| Difficulty swallowing (dysphagia), or jamming food |
| Painful swallowing (odynophagia) |
| Permanent hoarseness (laryngitis) |
| Feströker cough, newly discovered asthma, or asthma only at night |
| Pain in the stomach (pain in the upper abdomen) |
| The feeling of “lump” in the throat |
| Deterioration of dental disease |
| Frequent lung infections (pneumonia) |
| Chronic sinusitis |
| Waking up with a sense of strangulation |
The following signs and symptoms may indicate a more serious problem when the person should immediately consult a specialized physician:
| Alarming symptoms in patients with GERD |
|---|
| Difficult or painful swallowing (feeling that food gets “stuck”) |
| Unexplained weight loss |
| Chest Pain |
| Choking |
| Bleeding (vomiting blood or black stools phenomenon) |
Some people who suffer from GERD have no visible damage to endoscopic mucosal esophagus (non-erosive reflux disease, functional heartburn), while others have a clearly visible damage or complications (esophagitis, peptic strictures, Barrett’s esophagus) or have extraesophageal events in mind pulmonary, ear, pharyngeal or laryngeal symptoms. More details about the symptoms of GERD look into SYMPTOM AND.
Diagnostic
It is not necessary nor practical to start a detailed diagnosis in all patients with a feeling of heartburn. Acid Reflux is usually diagnosed based on symptoms and response to therapy. Treatment in the form of changes in living habits with the use of drugs, in some cases, are often recommended without further testing.
Indications for endoscopic examination of patients with GERD are very frequent and prolonged heartburn accompanied by regurgitation, difficulty swallowing, cough, or lung problems. A special group of patients are those in which began empirical therapy but with unsatisfactory results. Specific testing is required when the diagnosis is unclear or when there are more serious signs or symptoms previously mentioned. It is important to turn off potential life-threatening problems that can cause symptoms similar to those of GERD. This is especially true of chest pains, because he can be a symptom of heart disease or lung cancer. When symptoms are not life-threatening and diagnosis of GERD is not entirely clear, recommended a number of diagnostic tests.
In the diagnosis of GERD is necessary to distinguish this disease from infectious, caused by drugs and eosinophilic esophagitis, followed by peptic ulcer disease, non-ulcer dyspepsia, biliary disease (because it is important in the diagnosis of always to make echo-sonography of the abdomen) and motor disorders esophagus. Only on the basis of classical simtpomatologije often not possible to make a distinction between these diseases, so it is necessary to proceed to a detailed diagnosis. It is important to note that severity and duration of the actual symptoms of GERD in most cases are not directly correlated with the severity and degree of esophagitis. For patients with carcinoma conduct a thorough diagnostic evaluation is necessary to make endoscopy, esophageal pressure gauges as well as a 24-hour impedance / pH meter. All these diagnostic procedures offer very different but mutually significantly related information.
Radografija with double contrast is of limited value in the diagnosis of GERD because it has a very limited sensitivity in patients with milder forms. The biggest benefit of radiographic diagnosis in detecting peptic narrowing and large hiatal hernia. When comparing the results barium enema radiography and endoscopy, a diagnostic accuracy of radiography is 25% for a mild form of esophagitis, 82% for intermediate and 99% for severe esophagitis.
Esophagogastroduodenoscopy with biopsy if necessary, should be the initial diagnostic procedure when suspected GERD, because it is able to determine the further course of diagnosis and treatment. However, the lack of a typical endoscopic findings of GERD does not exclude the very existence of GERD. Sometimes patients with negative endoscopic findings during monitoring may develop damage to mucous membranes. On the other hand it is important to understand that the typical symptoms of GERD can sometimes be caused by hypersensitivity (hypersensitivity) of the esophagus. In determining the degree of inflammation of mucous membranes of the esophagus reflux gastric contents of today’s most frequently used Los Andjelos-to classification. This classification graded severity of esophageal inflammation (esophagitis) based on the extent of damage to the mucous membranes. For details, see chapter Diagnostics – Endoscopy of the upper digestive tract .
The significance of esophageal manometry in the diagnosis of GERD in the evaluation of esophageal peristaltic function of the body and pressure values of DES, primarily to assess the decision about the future form of treatment. In the case of basal tone DES extremely low and when there is significantly weakened peristalsis of the body of the esophagus as a result of chronic reflux, you need to think about antireflux surgical treatment. The importance of manometry is reflected in the precise determination of the place of DES to be placed in the most objective way to probe for a 24-hour impedance / pH meter. Details on the importance and techniques ezofagelane manometry look intoDIJAGNOSTIKA- esophageal manometry .
Implementation of 24 hour impedance / pH monitoring is useful to verify the GERD in patients with continuous symptoms (either typical or atypical) in which there is damage to the mucosal seen endoscope or the presence of large hiatal hernia, especially in cases where the effect of drug therapy inappropriate. This kind of diagnosis can also be used to monitor the effect of the applied therapy in patients with persistent symptoms. Details about this procedure, refer to section Diagnostics – 24 hour pH monitoring and impedance .
Complications
All of the complications of gastroesophageal reflux disease can be divided into three major categories:
- Inflammatory: esophagitis and esophageal ulcer.
- The consequences of scar / reparative processes esophagitis: peptic strictures and Barrett’s metaplasia.
- Extraesophageal event.
Most patients with gastroezofagelanom reflux disease will not develop serious complications, particularly when reflux is adequately treated. Beneficial, but the number of serious complications can rise in patients with long expressive GERB.
| GERD | ||||
|---|---|---|---|---|
| Prevalence (%) | 7.8% | 15% | 18% | 12.6% |
| % Of the population> 60 years. | 21% | 21% | 20% | 16% |
| The incidence of esophagitis | 20% | 20% | 20% | 20% |
| The incidence of peptic including wall | 10% | 8% | 10% | 8% |
| Incidence B arrett a | 12% | 12% | 10% | 12% |
| Incidence adeno at B arrett a | 8% | 8% | 8% | 8% |
The most common complication of GERD is the existence of reflux (peptic) esophagitis, or inflammation of mucous membranes of the esophagus uzrkovano effect of hydrochloric acid and duodenal contents on the final part of the mucous membrane of the esophagus. Patients with these complications generally have significant hiatal hernia, and the degree of damage is divided into four main groups depending on the severity of mucosal damage. Also, as a special form of complications of GERD can occur rarely and ulcers (ulcers in the esophagus). In some cases, with an ulcer in the esophagus, can occur more pronounced bleeding. Patients may not be aware of bleeding, but it can be detected in a stool sample test on occult bleeding.
Peptic narrowing (stenosis) of the esophagus is the result of healing esophagitis. Ošetećenje acid can cause scarring and narrowing of the esophagus which can lead to jamming of food and medicine in the esophagus. The narrowing is caused by scar tissue resulting from chronic inflammation of the terminal part of the esophagus, or when the damage occurs repeatedly and esophageal mucosal healing itself. Constriction are generally short in length and localized at or below the esophagogastric junction. Endoscopy can also be seen surrounding fields reflux esophagitis. The main symptom of this disease is dysphagia for solids and intermittent obstruction of the esophagus.
Gastroesophageal reflux followed by regurgitation and / or aspiration of gastric contents is often associated with extraesophageal complications such as asthma, laryngitis, chronic cough, erosion of teeth, chronic sinusitis, repeated pneumonia, chronic hoarseness, pharyngitis, and cancer of the larynx. Epidemiological data show that between 40 and 90% of people who suffer from asthma have GERD, while 40% of asthmatic patients have endoscopic findings of reflux esophagitis.
 ENT complications of GERD may also arise due to the reflux of gastric contents with consequent damage to the mucous membranes of the throat and larynx. The concept of laryngopharyngeal reflux is used to explain the process. Some people are acid reflux and throat, causing inflammation of the vocal cords, sore throat or hoarseness. The acid can be inhaled into the lungs and cause a specific type of ignition (aspiration pneumonia). Feströker acid reflux into the lungs potenijalno can cause permanent damage to the lungs, called pulmonary fibrosis or bronchiectasis.
ENT complications of GERD may also arise due to the reflux of gastric contents with consequent damage to the mucous membranes of the throat and larynx. The concept of laryngopharyngeal reflux is used to explain the process. Some people are acid reflux and throat, causing inflammation of the vocal cords, sore throat or hoarseness. The acid can be inhaled into the lungs and cause a specific type of ignition (aspiration pneumonia). Feströker acid reflux into the lungs potenijalno can cause permanent damage to the lungs, called pulmonary fibrosis or bronchiectasis.
Of all the complications of GERD is the most significant occurrence ofBarrett’s esophagus , which occurs when, because of long-standing chronic acid reflux into the esophagus, the normal cells lining the distal esophagus (pločastoslojevita mucous membranes) replacing the other type of cell (cylindrical – intestinal mucous membranes). This process usually occurs repeatedly in damage to the mucosa of the esophagus, and is usually caused by long-term gastroesophageal reflux disease. Intestinal cells have a low risk of transforming into malignant cells. Therefore, people with Barrett’s esophagus are recommended periodic control endoscopy in order to monitor the early warning signs of cancer. There are two main types of esophageal cancer, squamous cell carcinoma and adenocarcinoma. The largest risk factor for adenocarcinoma is Barrett’s esophagus. Unfortunately, adenocarcinoma of the esophagus is the last two decades the world has the greatest increase in incidence among all solid tumors.
Diseases
- Anatomy and Physiology of the Foregut
- Gastroesophageal Reflux Disease (GERD)
- Barrett’s Esophagus
- Hiatal Hernias
- Achalasia
- Esophageal Motility Disorders
- Esophageal Diverticula
- Helicobacter pylori gastritis
- Peptic Ulcer Disease (PUD)
- Gallstones (Cholelithiasis)
Lexicon
Patients Informations
Soon
If you have more questions contact us:
info@refluxcentar.com

 српски
српски