Helicobacter pylori gastritis
Gastritis is a term that refers to inflammation of the stomach.It is manifested as a feeling of aching pain, discomfort during and after meals, early fullness and slow digestion of the food.The discovery of the bacteria Helicobacter pylori, which often colonize the stomach has improved knowledge on the etiology and treatment of gastritis. Today It is believed that almost 2/3 of the world’s population is infected with H. pylori, but the vast majority have no symptoms and shall never because of it have any problems.On the other hand, H. pylori is able to create a number of problems in the digestive tract, including stomach and duodenal ulcers, but also significantly less gastric tumors (lymphoma and cancer).It is still not clear why certain patients get sick and others do not due, to the presence of H. pylori.H. pylori infection is most likely spread by consuming water or food contaminated by fecal matter.In addition to H. pylori gastritis may be caused by the use of nonsteroidal anti-inflammatory drugs, alcohol, and rarely occur as a result of an autoimmune process.
For details about the reasons of appearance, symptoms and diagnosis of gastritis read below.
Introduction
Gastritis is a term that refers to a group of pathologies which have one thing in common: inflammation of the mucous membrane of the stomach.This inflammation is the most common (˃ 80%) caused by a bacterium that colonizes the stomach lining and decreases its defensive capability.This bacterium called Helicobacter pylori (H. pylori) in spite of gastritis is also responsible for the creation of the largest number of ulcers in the duodenum and stomach.Ulcers can create a wide array of symptoms, or to be fully asimtpomatični.Helicobacter pylori is the most common bacterial infections in humans and may be in any part of the world of all ages.The second most common reason for the occurrence of gastritis (15%) was taking painkillers, so-called non-steroidal anti-inflammatory drugs (NSAIDs) such as diclofenac, ibruprofen and others.Aspirin also can lead to significant inflammation of the gastric mucosa.Apart from these, other risk factors for the occurrence of gastritis are: age (chronic gastritis is more common in the elderly), stress, excessive alcohol consumption, and chronic korikosteroidna therapy.
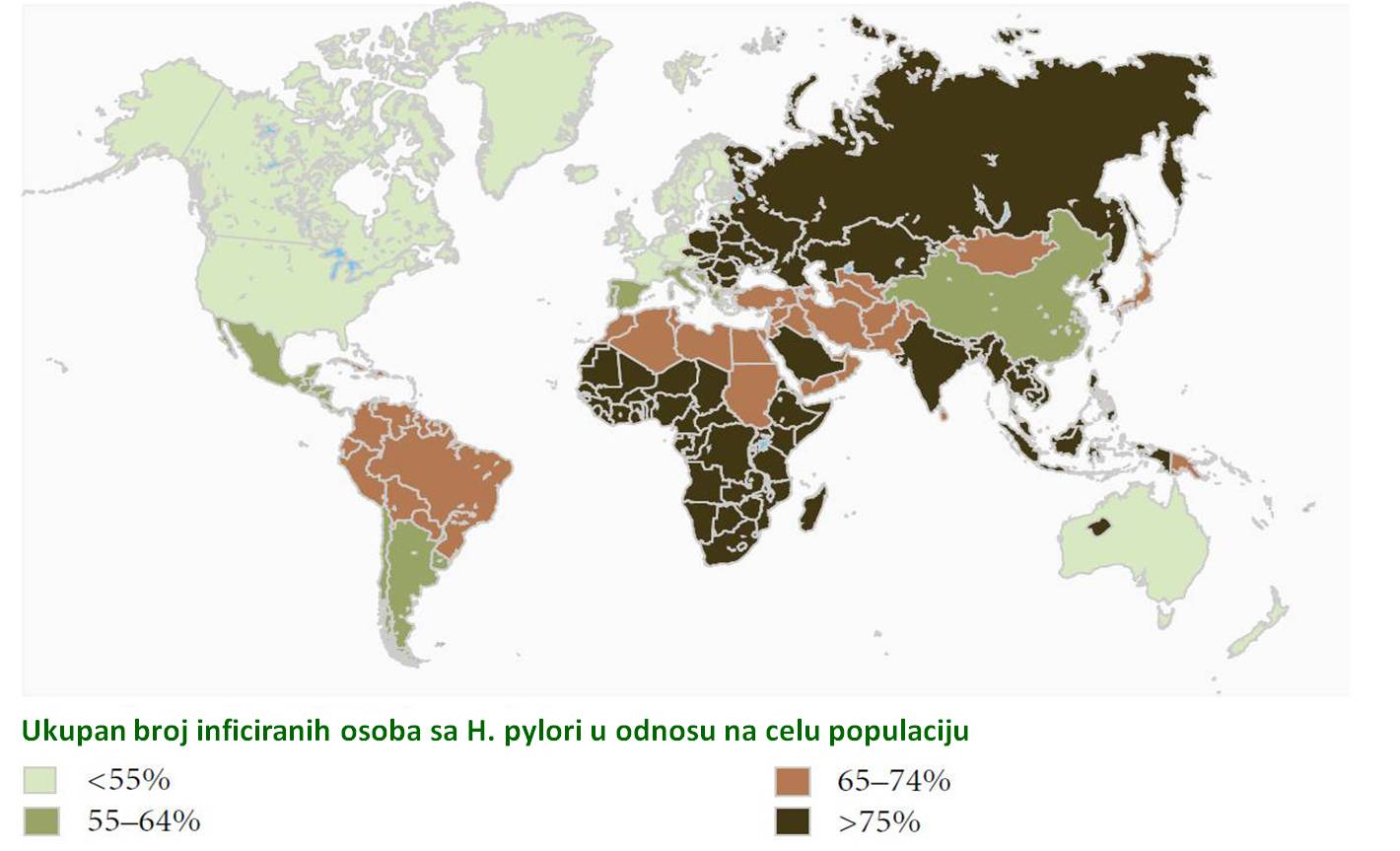
The prevalence of infection with H. pylori increases with age-age and socio-economic factors determine the age of acquisition of infection.Today, the prevalence of H. pylori infection in North America and Europe about 60%.Early treatment of infection is important because acute form usually eventually turns into chronic gastritis, on the ground that can be developed intestinal metaplasia in the stomach, which is a precursor to cancer development.The route of infection with H. pylori is not yet fully known, but the most common ways to transfer the fecal-oral (contaminated water), gastro-oral (person to person), oral-oral (dental plaque) and iatrogenic.It is now thought that if one parent has an infection with Helicobacter pylori, the child will be infected at about 40%, and the spouse in about 70% of cases.
Detection of Helicobacter pylori created a new classification system gastritis formed on the basis of topographical and morphological changes in the stomach, but with special emphasis on the etiology.
| The classification of gastritis (Sydney classification) | |
| Type gastritis | Acute |
| Feströker | |
| Specific (hypertrophic, eosinophilic) | |
| Localization | Antrum |
| Corps | |
| Pangastritis (full stomach) | |
| Etiology | Bacterial (Helicobacter pylori) |
| Non-bacterial (NSAIDs, alcohol) | |
| Unknown | |
| Morphology | inflammation, atrophy, intestinal metaplasia, Helicobacter pylori (colonization density) |
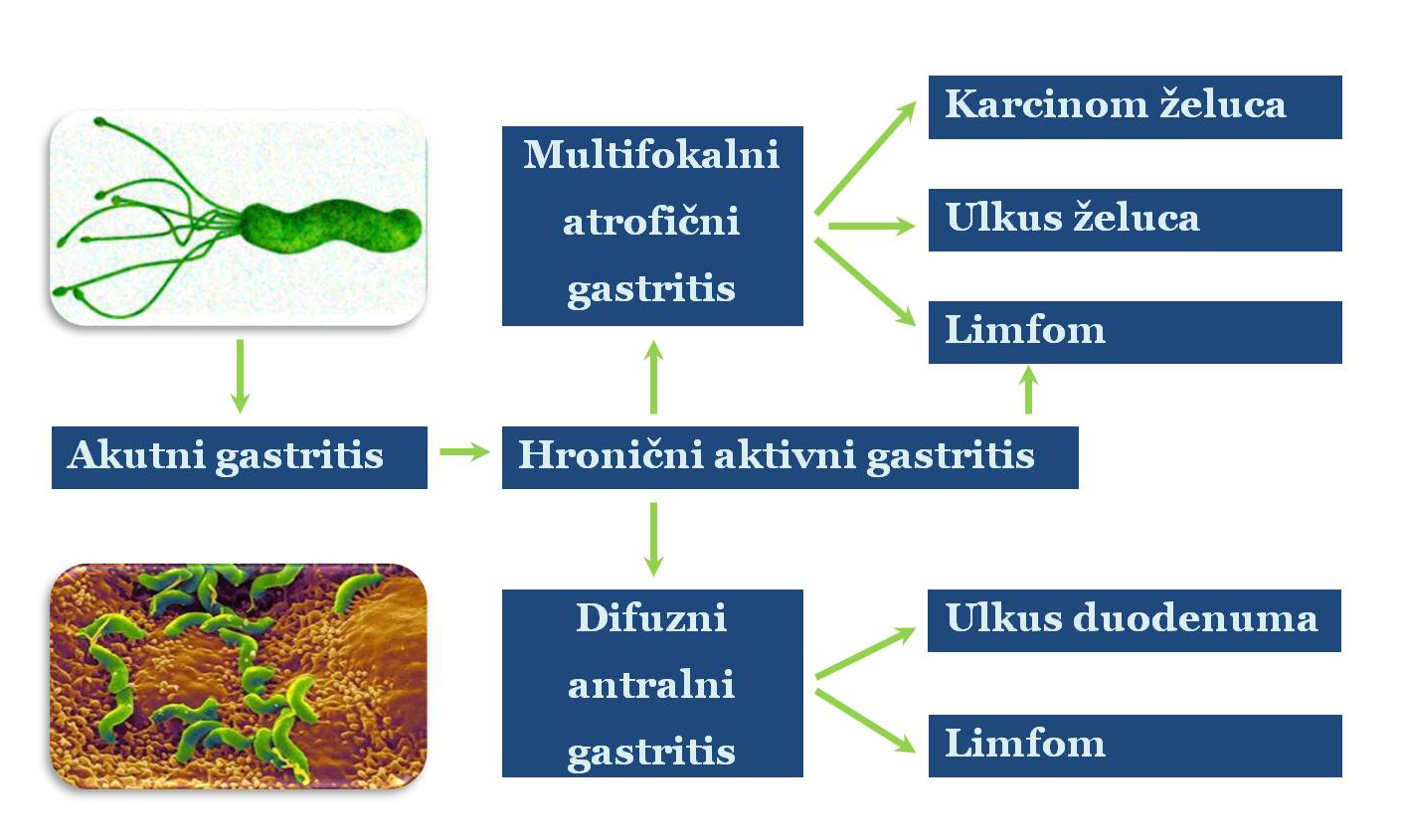
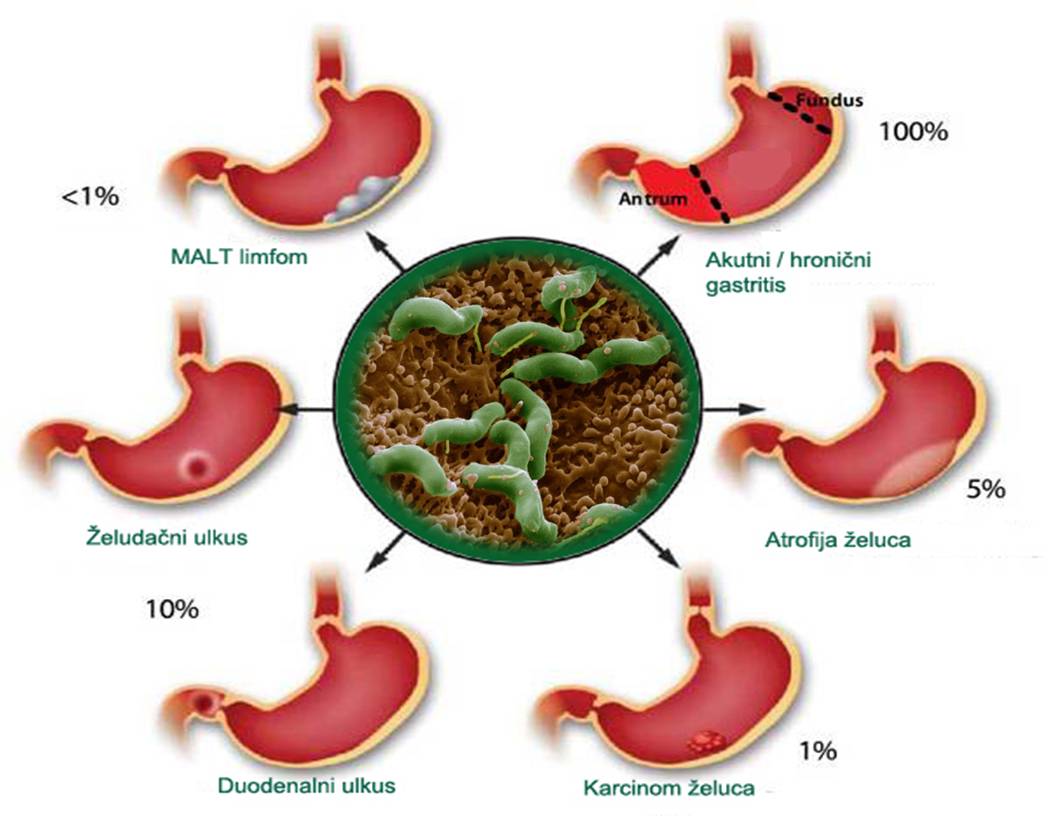
Gastritis was due to Helicobacter pylori infection can arise suddenly, and it is called acute, or occurs gradually over time and it is called chronic gastritis.Chronic active Gastrīts be in yavisnosti of distribution divided into two groups: diffuse antral gastritis DAG (surgery only when the final part of the stomach) and multifocal atrophic gastritis (MAG procedure when the whole superficial stomach).In patients who have a DAG may occur duodenal ulcer or gastric MALT lymphoma, while in patients with a MAG can be developed ulcer, MALT lymphoma, or gastric cancer and.Generally infection with H. pylori can cause the following diseases: functional dyspepsia, diffuse antral gastritis, multifocal atrophic gastritis, gastroesophageal reflux disease, duodenal and gastric ulcer, gastric MALT lymphoma and gastric cancer.
H. pylori is present in the biopsy cause gastric mucosa in 90 – 100% of patients with duodenal and 70% with gastric ulcer, 80% of cases of chronic gastritis and 50% of people with functional non-ulcer dyspepsia.Of extreme importance to note that each ulcer it is necessary to thoroughly diagnose and closely monitored because there is a probability of malignant alterations, or the appearance of cancers based ulcers.If there is an infection with H. pylori chances of asymptomatic chronic gastritis is about 80%, atrophic gastritis with the advent of intestinal metaplasia around 20%, while gastric ulcer occur in less than 15% of cases.The incidence of the most serious diseases of the stomach MALT lymphoma and gastric cancer caused by infection with H. pylori is very small, and less than 1%.Despite the low incidence of occurrence, by the standards of the World Health Organisation of (WHO) and the International Agency for Research on Cancer (IARC) infection with H. pylori represents carcinogen class in the occurrence of gastric cancer (the same as tobacco for lung cancer or hepatitis to liver cancer ).
Nonsteroidal anti-inflammatory drugs (NSAIDs), diclofenac and ibuprofen, and aspirin are the most common used drugs in the world and represent after H. pylori infection and the most common cause of gastritis and gastric ulcer formation.In Europe, every day about 30 million people use NSAIDs as well as about 20% of US residents over the age of 70 years.Due to the widespread use of a large number of complications and side effects of these drugs have become a significant medical problem.Patients who for a long time and regularly using NSAIDs have frequent small superficial bleeding in the stomach in about 50% appear small erosion (damage to gastric mucosa), while a stomach ulcer due to severe forms of gastritis developed in 15% of cases.Most of these lesions (80%) passes asymptomatically.The annual risk of serious complications such as bleeding in patients with chronic NSAID therapy is about 3%.The risk of ulcers in these sufferers is higher in the elderly and people suffering from rheumatoid arthritis.
However, the vast majority of patients with gastritis after adequate therapy usually recovers quickly.Regular monitoring is recommended in these patients, as well as specific dietary regime.
Symptoms
The most common symptom of gastritis is pain in the upper abdomen (epigastriujm) and below the right rib cage.The pain is dull in character, sometimes glowing, and patients often describe it as a feeling of discomfort in the stomach.If we look at them on the incidence of symptoms of gastritis are:
1. dull pain in the upper abdomen
2. feeling bloated after oborka and fast food saturation
3. Nausea
4. vomiting
It is important to note that symptoms of gastritis can sometimes occur with other diseases of the digestive tract, so it is the more frequent incidence of the symptoms listed above absolute indication for medical consultation.
Diagnostic
During the first fast doctors, diagnostic process begins by talking and taking important data on your current condition.The doctor will usually ask you some of the following questions:
1. How have expressed your symptoms, and would you describe abdominal pain as discomfort or burning?
2. Are your symptoms constant or intermittent?
3. Does the stomach pain occurs immediately after a meal or after 2-3 hours?
4. Does the taking of special foods leads to worsening of symptoms?
5. Does the consumption of some foods or taking antacids reduces your problems?
6. Do you have nausea or vomiting?
7. Have you lost any weight?
8. Do you take painkillers or anti-clotting?
9. Have you recently consumed alcohol more often?
10. In the list under chronic or acute stress?
11. Do you set prior history of ulcer, or someone in your family had an ulcer?
12. Have you noticed a black stools, vomiting or bloody content?
After a detailed interview and clinical examination, the doctor will suggest a number of diagnostic procedures:
1 contrast Radiological examinations of the stomach and duodenum – a limited role in the diagnosis of gastritis, and low specificity and sensitivity, but is useful in the detection of disorders of the stomach materials or in evaluation of gastric emptying (fluoroscopically)
2. Abdominal ultrasound – also has no significant role in diagnosis of gastritis, but is useful in the detection of possible associated pathological conditions, such as, for example, calculosis gallbladder which sometimes can lead to similar symptoms of gastritis
3. gonjeg digestive tract endoscopy – the procedure is the gold standard for diagnosis of gastritis.This examination can directly visualize the stomach lining and already seen the emergence of the earliest signs of inflammation, such as redness and swelling (edema) of mucous membranes.Also, when endoscopy is possible to take a biopsy of mucous membranes, and thus through histology accurately confirm and define a subtype of gastritis, or possibly detect the presence of Helicobacter pylori infection, which as already mentioned, the prime cause of gastritis and wider at the stomach and duodenum.
Detection of Helicobacter pylori and it is often the first step in the treatment of gastritis.There are several different ways of determining the presence of H. pylori infection.This can be achieved by determining the presence in the serum anititela (by taking blood, estimated to be of IgA and IgG anititela), then breath test (Urease breath test), faecal analysis and the aforementioned endoscopic biopsy.It is believed that the breath test and endoscopic biopsies have the highest sensitivity and specificity in determining Helicobacter pylori infection (95%), while the diagnostic value of determining antibodies fekanlnom analysis of smaller (<90%), and the blood is limited, with frequent false positive and negative results (80%).
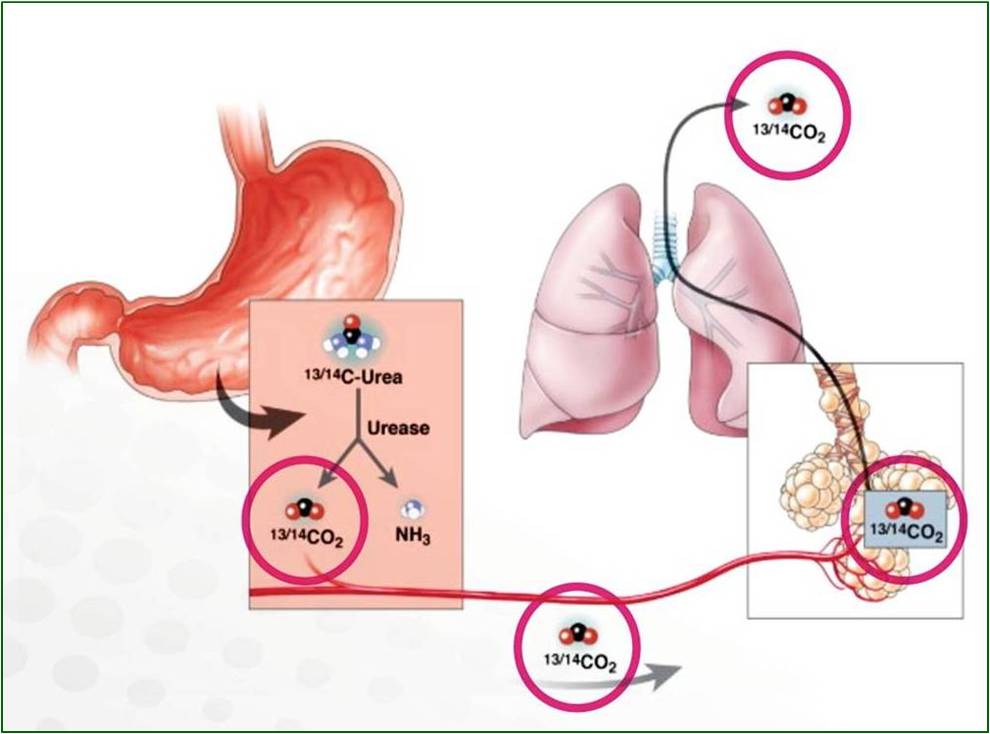
Breath test for the determination of Helicobacter pylori infection
Breath test for Helicobacter pylori has been formed on the basis of the fact that this bacterium produces the enzyme urease, which decomposes urea given orally, which is then decomposed by hydrolysis.One of the products of urea is razdradnje CO2 eliminates through the lungs and is present in the exhaled air.If the carbon (C) in the preparation of urea active bookmark, it can be detected in the air izdahutom and accurately determine the presence of Helicobacter pylori infection.
During the test, the subjects were given to drink composition comprising a urea with activated carbon (C-14).If H. pylori is present on the urea decomposes in the exhaled air will, after 30 minutes to be present C-14, so that the result is obtained very quickly.
To review results were reliable, it is necessary that the patient does not eat 6 hours before the examination (individual foods may contain substances that interfere review).Also, drugs that block acid secretion from the stomach affect the results of the inspection, so that they should be suspended for at least 14 days prior to performance reviews.These drugs are proton pump inhibitors (eg. Nexium, Controloc) and H2 receptor blockers (e.g., Ranitidine, Famotidine).Also, the review should be postponed at least a month of antibiotics.
A properly conducted breath test in assessing the Helicobacter pylori infection has a high reliability, and is considered to be almost equivalent to the histopathological findings obtained by endoscopic biopsy.The test is snug to the patient, no side effects, easy and the results are obtained quickly.
Diseases
- Anatomy and Physiology of the Foregut
- Gastroesophageal Reflux Disease (GERD)
- Barrett’s Esophagus
- Hiatal Hernias
- Achalasia
- Esophageal Motility Disorders
- Esophageal Diverticula
- Helicobacter pylori gastritis
- Peptic Ulcer Disease (PUD)
- Gallstones (Cholelithiasis)
Lexicon
Patients Informations
Soon
If you have more questions contact us:
info@refluxcentar.com

 српски
српски